Social Prescribing in The USA: On the Rise?
What is social prescribing? What if, when a patient went to their health care provider for an ailment like depression, their provider not only offered pharmaceutical and clinical solutions, but asked about their interests and passions? And, after a person-centered discussion, the provider recommended and referred the patient to a community gardening class, or to join a local group that regularly goes on walks and hikes?
Or, if someone who is experiencing high cholesterol received a referral to a nutritionist, and a voucher to attend a cooking class focused on healthy, easy to make meals at home, instead of vague advice on “being more active” and possible prescriptions for weight loss pills?
This is social prescribing. It shifts the questions providers ask away from “What is the matter with you?” to “What matters to you?” Social Prescribing is on the rise globally, particularly in Europe, but hasn’t been fully embraced in the United States just yet.
A Prescription for Wellness
Social prescribing is born from the understanding that not all ailments or factors impacting an individual’s health can be addressed through traditional medicine, or in the brief amount of time an individual is actually in a doctor’s office. Aimed largely at prevention, social prescribing bridges the worlds of clinical and community health, supplements traditional care methods, and allows the patient or client to bring their interests and assets to the table to further their own health goals.
The United States has been slow to adopt the social prescribing ideology, but that may change quickly; mental health issues like social isolation and loneliness have reached crisis levels in the US, especially among young people, adolescents, and older adults. Read on to see how Europe is leading the way, and how the U.S. is slowly adopting social prescribing.
Social Prescribing in Europe
European countries like Ireland, Scotland, and England have been ahead of the curve on social prescribing. Large-scale government programs are currently underway that feature social prescribing as a means to address mental and physical health concerns. Initiatives such as England’s National Health Service’s Long Term Plan, launched in 2019, is aimed at shifting NHS’ priorities and funding into a more “universal personalised care” model. Universal personalized care gives people the “same choice and control over their mental and physical health that they have come to expect in every other aspect of their life.”
Link workers are an integral part of NHS’ plan, and serve as a linchpin to resource referrals.
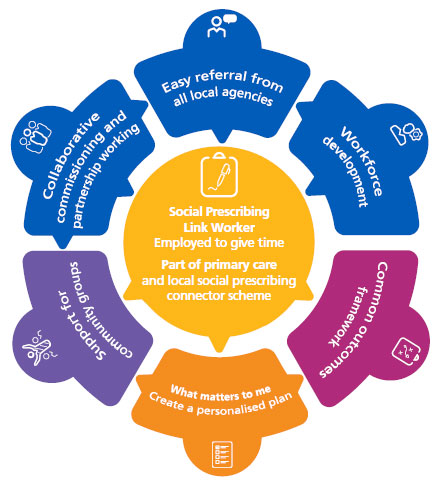
NHS’ Social Prescribing Model.
Doctors refer their patients to link workers for a variety of care needs, and link workers take it from there, helping and linking patients to appropriate resources in the community. Doctors play a large role in directing patients to link workers, but many other entities can refer people to link workers as well, such as pharmacies, fire and police departments, job centers, social services, and community organizations. People are also encouraged to refer themselves to a link worker.
If key components are successfully implemented, the NHS expects the plan to benefit over 2.5 million people by 2023/24. Some key objectives:
- Helping to train and evolve the existing skills of 75,000 health professionals and clinicians to use a more personalized care approach in their regular practice;
- Train and implement over 1,000 link workers to refer people to social prescribing, with hopes that over 900,000 people will be referred by 2023/24;
- Give 200,000 people the power to customize their health care by giving them a personal health budget, which aims to improve their experiences with the system by giving them greater involvement and choice
Beginning in 2021, the European Union’s Horizon Europe program, is a €95 billion, six-year investment seeking to bolster research and development, innovation, and entrepreneurship. Horizon Europe provides over 90% of the funding to the RECETAS project, which is currently active, and taking place in six cities across Europe, Latin America, and Australia. RECETAS is an acronym for Re-imagining Environments for Connection and Engagement: Testing Actions for Social Prescribing in Natural Spaces, and as the name suggests, it takes social prescribing to the outdoors; it encourages residents of dense urban areas to get out into nature, as it “can provide therapeutic benefits and promote social interaction.”
Visible Network Labs is proud to be the exclusive American partner in the RECETAS project, working to provide our network science expertise, as well as our PARTNER Community Partner Relationship Management (CPRM) tool to organizations in cities around the world to help them better understand their networks and their reach. More details and information on our participation in this innovative and exciting project is coming soon.
Social Prescription in the U.S.
In North America, Canada has embraced the use of social prescribing. Yet social prescription, as it is more commonly referred to in the U.S., is currently limited, especially at a federal and state level. One of the first government initiatives to rise to prominence is Compassionate Care Corps, a tele-support program run by the Department of Veterans Affairs.
If veterans are feeling isolated, lonely, or just want to engage in regular conversation, they can talk to their clinician or advocate to receive a referral to the program, which connects them to a volunteer. Most volunteers are from veteran service organizations, and many are veterans themselves. Training for volunteers covers topics like compassion, empathy, support, privacy, and confidentiality, and screeners are used to match veterans with volunteers who have similar interests. Around 1,000 veterans are participating, and over 100 VA sites are utilizing the program.
U.S. Surgeon General Murthy
U.S. Surgeon General Murthy Testifying at a Senate Finance Committee Hearing.
Even before the onset of the pandemic, U.S. Surgeon General Vivek Murthy has been calling attention to the rise of isolation and loneliness in the U.S., its role as a social determinant of health, and its impacts on mental and physical health.
Surgeon General Murthy published a book, titled Together: The Healing Power of Human Connection in a Sometimes Lonely World on April 7th, 2020, right as many Americans were experiencing profound, yet necessary isolation. Dr. Mark Hyman, head of Strategy and Innovation at the Cleveland Clinic for Functional Medicine, says of the book: “An invisible crisis plagues America today. It’s responsible for more sickness, suffering, and death than almost anything else. It is loneliness. It is often underneath addiction, suicide, and even obesity.”
On December 7th, 2021, Surgeon General Murthy released an Advisory, titled Protecting Youth Mental Health. In the advisory, addressing what health care providers can do to help, Surgeon General Murthy says “Recognize that the best treatment is prevention of mental health challenges … health care professionals should work with other sectors (e.g., schools, child care, justice, social services, public health) on prevention strategies…health care professionals can refer patients to resources such as economic supports, school enrichment programs, and legal supports.”
The Future of Social Prescription in the U.S.
As we emerge from an unprecedented period of social isolation, the need for innovative ways to reconnect society and rebuild networks are more important than ever. With endorsements from officials like Surgeon General Murthy, adoption by federal agencies such as the VA, and an established playbook from programs in Europe and around the world, social prescription is likely to expand as an effective and economically viable prevention and treatment measure in the United States in the coming years.
Be sure to stay tuned to our Visible Us Blog for more product updates and VNL Team content!
About the Author: Will Jacobson
Will Jacobson is the Business Development Representative on VNL’s Marketing and Communications Team. Originally from New York City, Will loves living in Colorado and all the outdoor life it has to offer. He’s also a pretty big foodie!
|
|
Thank you for Signing Up |

More Social Care Resources